Oxygen is the most essential element for life and without oxygen humans can survive for a few minutes only. The adverse consequences of hypoxia are well known, so it’s surprising to many to hear that controlled exposure to oxygen deficit (or hypoxia) if within a person’s adaptive range, can actually promote longevity, enhance physical performance and even help to create conditions that support healing in certain diseases (Serebrovskaya 2002, Verges, Chacaroun et al. 2015). There should be a balance between oxygen demand and delivery in order to maintain homeostasis within the body.
Nobel Prize 2019 – Oxygen sensing decoded
The 2019 Nobel Prize in Physiology or Medicine was awarded to three physician scientists, Drs. William G. Kaelin, Jr., Peter Ratcliffe and Gregg Semenza, for their groundbreaking work revealing how cells sense and adapt to oxygen availability. Oxygen is vital for all living organisms. During the course of evolution, animals have developed the ability to adapt to changes in the oxygen concentration on earth. However, it was unclear how animals can sense and adapt to changes in oxygen availability until around thirty years ago.
More information https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6889041/
 For their discoveries of how cells sense
For their discoveries of how cells sense
and adapt to oxygen availability
How cells sense and adapt to oxygen availability
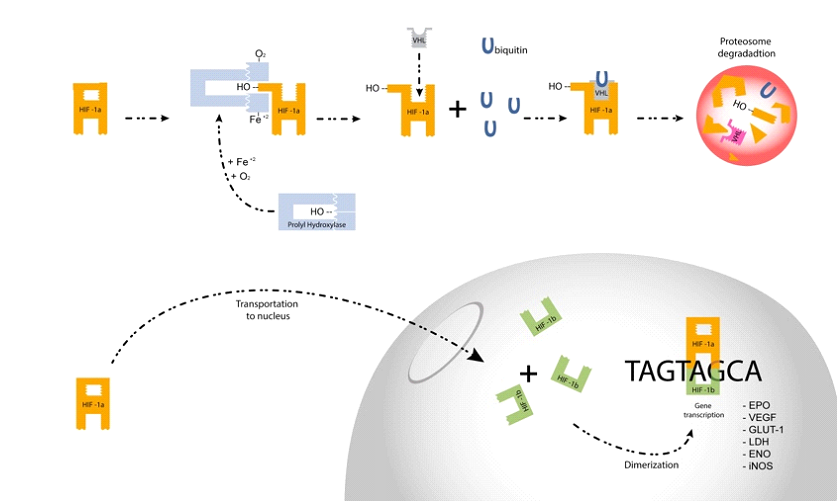
Hypoxia-inducible factor 1 (HIF-1) is an oxygen-regulated transcriptional activator that plays essential roles in mammalian development, physiology and disease pathogenesis… HIF-1 is ubiquitinated and subjected to proteasomal degradation in non-hypoxic cells.
Under hypoxic conditions, the fraction of HIF-1 that is ubiquitinated decreases dramatically, resulting in an accumulation of the protein https://pubmed.ncbi.nlm.nih.gov/11248550/
THE KEY REGULATORS OF O2 DELIVERY AND UTILIZATION
Hypoxia Inducible Factors – the key regulators of o2 delivery and utilization
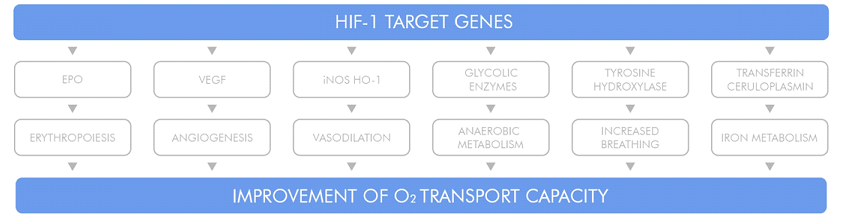
- HIF-1 controls oxygen delivery, by regulating angiogenesis and vascular remodeling, as long as oxygen utilization, by regulating glucose metabolism and redox homeostasis;
- HIF-1 activity is induced by hypoxia through changes in HIF-1α mRNA and protein levels in brain, heart, kidney, lung and skeletal muscle;
- HIF-1 functions as a master regulator in angiogenesis and vascular remodeling process because it coordinately regulates the expression of a large number of genes whose protein products play critical roles in mediating vascular responses to hypoxia and ischemia;
- Normal physiological response to reduced tissue perfusion is that the resulting tissue hypoxia induces HIF-1 activity, which activates transcription of genes encoding angiogenic factors. These factors stimulate the remodeling of collateral blood vessels, leading to increased blood flow.
- In addition to promoting O2 delivery, HIF-1 also activates the transcription of genes encoding enzymes, transporters, and mitochondrial proteins that decrease O2 utilization, again functioning as a master regulator to switch cells from oxidative metabolism to glycolytic metabolism